Individualized, Multidisciplinary Approach to Pain Management Is Needed, HHS Task Force Chair Tells KCMS Annual Meeting
Dr. Singh chaired the federal Pain Management Best Practices Inter-Agency Task Force that released its report on pain management best practices in May. She chaired the task force as part of her work as chief medical officer for the Office of the Assistant Secretary for Health, U.S. Department of Health & Human Services, from June 2017 through July 2019. Dr. Singh also has served at Stanford University School of Medicine for the past 13 years as clinical associate professor of anesthesiology, perioperative and pain medicine.
“Pain matters. Addressing it matters. How we address pain is what enables people to recover and return to society. It has to remain at the forefront of what we do,” Dr. Singh said.
(click on image to enlarge)
Data from the Centers for Disease Control and Prevention show that some 50 million American adults suffer from chronic pain daily or almost daily, and 19.6 million American adults have high-impact chronic pain that significantly affects their quality of life, she quoted from the task force report. This in turn has led to the opioid crisis where people becoming addicted to prescription painkillers, and then end up obtaining substitutes on the street that often are laced with the much more powerful and damaging fentanyl.
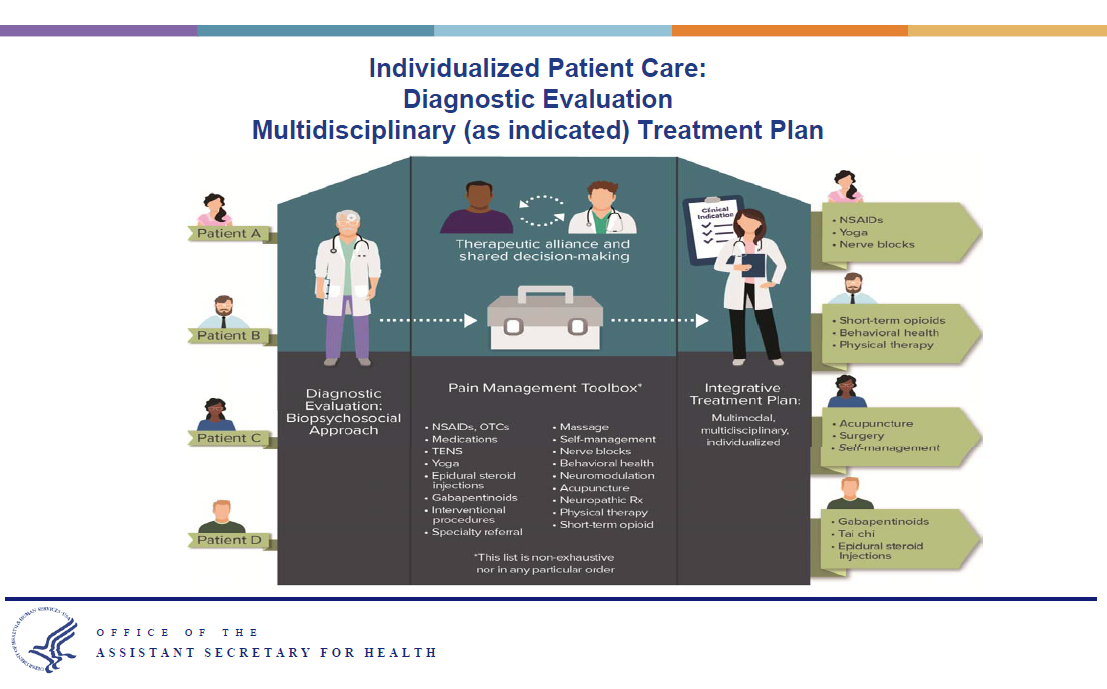
Dr. Singh presented the model for pain management proposed by the task force.
In assessing the patient, the task force calls for a biopsychosocial approach. The physician should consider three components: biological factors (age, injury, diagnosis, general health), psychological factors (mood, stress, trauma) and social factors (culture, education, spirituality). This provides a complete, holistic view of the patient.
(click on image to enlarge)
Treatment should be individualized, multimodal and multidisciplinary , she said. The mix available to the physician includes not just medications, but also can incorporate interventional procedures, restorative therapies, behavioral health, and complementary and integrative health approaches. The report details options in each of these areas.
“This pain management model places even greater priority on the physician-patient relationship,” Dr. Singh said. “Together they can arrive at a treatment plan that best suits the patient’s individual needs and circumstances.”
The task force had 29 members including representatives of federal agencies, hospital associations, medical organizations, patient advocacy organizations and others, along with experts in pain management, substance use disorder, primary care, pharmacy and other areas. The report was the result of broad stakeholder input including more than 10,000 public comments, she said. The report has been endorsed by the American Medical Association, the Association of American Physicians and Surgeons and many other organizations.
Follow the activities of the Pain Management Task Force through these links: